Why Are My Dog's Gums Pale? A Vet's Guide to Causes & Action
Here's a weird fact from the exam room: some dogs' gums are naturally pigmented dark, making it nearly impossible to assess gum color changes. So, knowing *your* dog's baseline is mission-critical. Don't assume that all pink gums are healthy gums, or that dark gums are necessarily a problem.
If your dog's gums are paler than usual, it means something is wrong. Pale gums, or pallor, indicates reduced blood flow or anemia. This can stem from various underlying conditions, some of which are life-threatening and require immediate veterinary attention. If you see pale gums, especially with other symptoms, seek veterinary help *immediately*.
How to Check Your Dog's Gums for Paleness
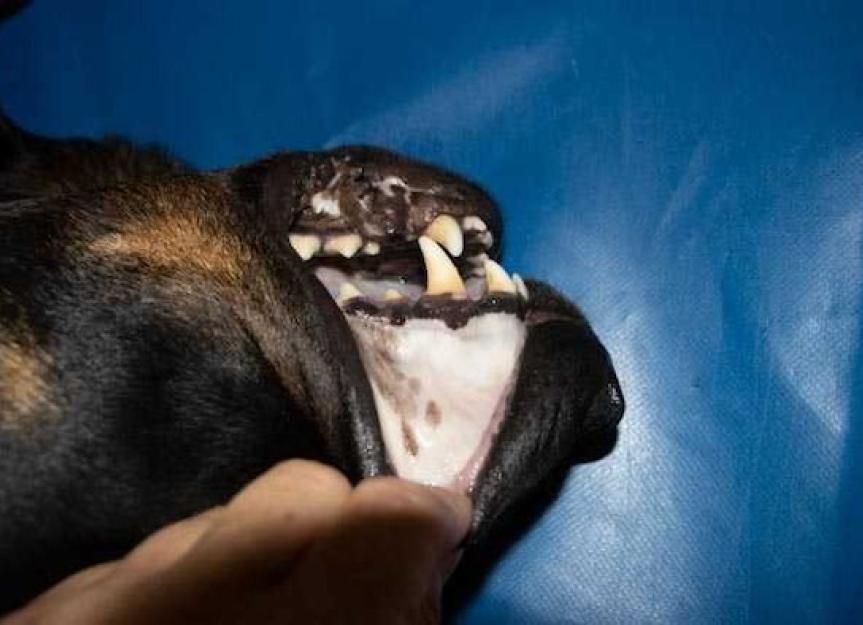
Normal, healthy dog gums should be a bubble-gum pink color. To check, gently lift your dog's upper lip. Do this regularly when your dog is relaxed. Any color change, like white, blue, or yellow, signals potential health problems that need veterinary assessment, STAT.
What Does Normal Dog Gum Color Look Like?
Normal dog gums should ideally be a shade of pink similar to that of cooked shrimp. Honestly, what I tell my clients is to check regularly so you KNOW what's normal for YOUR dog. Some dogs have naturally dark or even black gums due to pigmentation, but even in these cases, there are usually patches of pink that you can use as your baseline. The key is consistent monitoring.
To examine your dog's gums, gently lift their upper lip or pull down their lower lip when they are calm. I recommend doing this once or twice a month. This way, you establish a normal baseline. If you notice any deviation from this normal color—white, gray, blue, or yellow—it’s a non-negotiable sign that something is amiss.
The Clinical Perspective: Gum color reflects the perfusion of blood in the capillaries of the gingival tissue. Healthy gums are pink because red blood cells are carrying oxygen. Paleness indicates a reduction in red blood cells (anemia) or decreased blood flow (poor perfusion). Conditions like shock cause vasoconstriction, shunting blood away from peripheral tissues like the gums to protect vital organs, resulting in pallor. Other color changes are also significant, such as blue gums (cyanosis) indicating low oxygen levels in the blood.
Why Are My Dog's Gums Pale? Understanding the Root Causes
Pale or white gums in dogs are *never* normal and usually indicate an underlying medical problem that demands immediate attention. The most common reason is anemia, a deficiency in red blood cells. But here's the deal, anemia itself is just a symptom. We need to figure out *why* the dog is anemic. Poor circulation due to shock or underlying health problems can also cause pallor.
Here's a deeper look at the potential culprits:
- Immune-Mediated Hemolytic Anemia (IMHA): In IMHA, the dog's immune system goes haywire and starts destroying its own red blood cells. This can be triggered by drug reactions, vaccine responses, snake bites (especially copperheads or rattlesnakes-- I see this a LOT in the exam room in the fall). Sometimes, it's just primary immune system dysfunction.
- Internal Bleeding: Trauma, bleeding ulcers, tumors, clotting disorders, severe parasite infestations, or rat poison ingestion can all lead to significant blood loss. The loss of blood directly causes anemia.
- Shock: Shock is a life-threatening condition where the body doesn't get enough blood flow, leading to organ damage. It can happen fast and is often fatal without treatment.
- Toxins: Rat poison is a common culprit. Most rat poisons interfere with blood clotting, leading to internal bleeding. Early diagnosis is key.
- Heart Disease: Heart conditions like valvular disease, dilated cardiomyopathy, or congenital malformations can lead to congestive heart failure. This reduces oxygen delivery to tissues.
- Cancer: Some cancers cause bleeding tumors, most often found on the spleen, liver, GI tract, or kidneys. These tumors can rupture, causing acute bleeding.
- Clotting Disorders: Some dogs are born with clotting factor deficiencies, like Von Willebrand disease or Hemophilia A. Other causes include rat poison, cancers, or immune-mediated thrombocytopenia (low platelet count).
- Bloat (GDV): Gastric dilatation and volvulus (GDV) is when the stomach fills with gas and twists. This blocks blood flow and leads to shock.
- Parasites: Hookworm infestations can cause blood loss in the GI tract. Severe flea infestations can also cause anemia.
- Kidney Disease: Severe kidney disease can cause dehydration and affect red blood cell production.
- Severe Stress/Pain/Anxiety: Panting and nervous system activation can cause pale gums.
The Clinical Perspective: IMHA is a classic example of a Type II hypersensitivity reaction. Antibodies bind to the surface of red blood cells, marking them for destruction by the spleen and liver. This process is often mediated by complement activation, further amplifying the destruction. Some breeds, like Cocker Spaniels and Poodles, are genetically predisposed to IMHA, suggesting a role for specific MHC (major histocompatibility complex) alleles in disease susceptibility.
The Clinical Perspective: Internal bleeding leads to a drop in blood volume, causing hypovolemia. The body attempts to compensate by increasing heart rate and constricting blood vessels. Chronic blood loss can also lead to iron deficiency anemia, as the body depletes its iron stores trying to produce more red blood cells.
The Clinical Perspective: Shock disrupts cellular metabolism. Without adequate oxygen delivery, cells switch to anaerobic respiration, producing lactic acid and leading to metabolic acidosis. This acidosis impairs enzyme function and further compromises organ function. Prolonged shock can lead to irreversible organ damage and death.
The Clinical Perspective: Most rodenticides work by inhibiting vitamin K epoxide reductase, an enzyme essential for recycling vitamin K. Vitamin K is a cofactor for several clotting factors. Without it, the liver can't produce functional clotting factors, leading to uncontrolled bleeding.
The Clinical Perspective: Heart failure leads to reduced cardiac output, meaning less blood is pumped out with each beat. This triggers compensatory mechanisms like increased heart rate and vasoconstriction. However, these mechanisms eventually fail, leading to fluid buildup in the lungs (pulmonary edema) and tissues (ascites). The reduced oxygen delivery to the gums causes pallor.
The Clinical Perspective: Cancer cells can secrete factors that promote angiogenesis (new blood vessel formation) to support their growth. These new blood vessels are often fragile and prone to rupture. Some cancers also directly invade and erode blood vessels, leading to bleeding.
The Clinical Perspective: Clotting disorders disrupt the coagulation cascade, a complex series of enzymatic reactions that lead to the formation of a blood clot. Deficiencies in any of the clotting factors can prolong bleeding time and increase the risk of hemorrhage.
The Clinical Perspective: GDV obstructs blood flow to the stomach and other abdominal organs. The distended stomach compresses the caudal vena cava, reducing venous return to the heart. This leads to decreased cardiac output and shock. The twisting also causes ischemia (lack of blood flow) to the stomach wall, leading to necrosis (tissue death).
The Clinical Perspective: Hookworms attach to the intestinal lining and feed on blood. Chronic hookworm infestations can lead to significant blood loss and iron deficiency anemia. Fleas also feed on blood, and severe infestations can cause anemia, especially in puppies.
The Clinical Perspective: The kidneys produce erythropoietin, a hormone that stimulates red blood cell production in the bone marrow. In kidney disease, erythropoietin production decreases, leading to anemia. The buildup of uremic toxins in kidney disease can also suppress bone marrow function.
The Clinical Perspective: Stress and anxiety trigger the release of catecholamines (epinephrine and norepinephrine). These hormones cause vasoconstriction in peripheral tissues, leading to pallor. Panting can also cause dehydration, which can reduce blood volume and contribute to pallor.
What To Do if Your Dog Has Pale Gums and When to Seek Emergency Care
If your dog has pale gums, call your vet to schedule an appointment. If the gums are white or accompanied by other concerning signs, seek emergency veterinary care immediately.
Red Flag Checklist: Get to the ER if you see:
- Vomiting or diarrhea
- Black, tarry stool (melena)
- Severe lethargy
- Difficulty walking (ataxia)
- Weakness
- Collapse
- Trouble breathing
- Coughing
- Swollen stomach
- Bruising
- Bleeding
- Trauma
- No appetite
Home-Care Hacks: While waiting for your vet appointment (or on the way to the ER), keep your dog calm and quiet. Avoid strenuous activity. Make sure they have access to fresh water, but don't force them to drink. Note any other symptoms you observe, as this information will be valuable for your veterinarian.
How Do Vets Diagnose the Cause of Pale Gums in Dogs?
Speed is mission-critical. To find the underlying cause of pale gums, vets use a combination of tools:
- Thorough History: Knowing if your dog got into rat poison or has a heart condition is valuable.
- Physical Examination: A swollen stomach, breathing trouble, or bruising provide clues.
- Complete Blood Count (CBC): This blood test assesses red blood cells, white blood cells, and platelets.
- Serum Chemistry Panel: This blood test checks kidney and liver enzymes, glucose, proteins, and electrolytes.
- Urinalysis: A urine test checks for inflammation, infection, and abnormal cells.
- Chest Radiographs (X-rays): These images check for heart disease, lung bleeding, and cancer.
- Echocardiography: An ultrasound to check for heart disease.
- Abdominal Ultrasound: Visualizes abdominal organs for bleeding, tumors, or kidney changes.
- Coagulation Testing: Assesses how quickly blood clots.
- Fecal Testing: Checks for intestinal parasites and blood in the feces.
- Infectious Disease Testing: Checks for viruses, bacteria, and tick-borne diseases.
- Bone Marrow Aspiration and Biopsy: A more invasive test to investigate blood cell production.
How Do Vets Treat Pale Gums in Dogs and What is the Prognosis?
Treatment depends entirely on the underlying cause. Sometimes surgery is needed (bleeding tumors or bloat). Other times, antibiotics, antivirals, immunosuppressants, or steroids are necessary.
The Clinical Perspective: The prognosis varies widely depending on the underlying cause and the dog's overall health. IMHA can be managed with immunosuppressive drugs, but relapses are common. GDV requires immediate surgery to decompress and untwist the stomach. Cancer treatment depends on the type and stage of cancer. Rodenticide toxicity can be reversed with vitamin K injections if caught early.
The key takeaway? If you're concerned about your dog's gums, especially if they have other symptoms, see a vet ASAP. Early diagnosis and treatment can make all the difference.