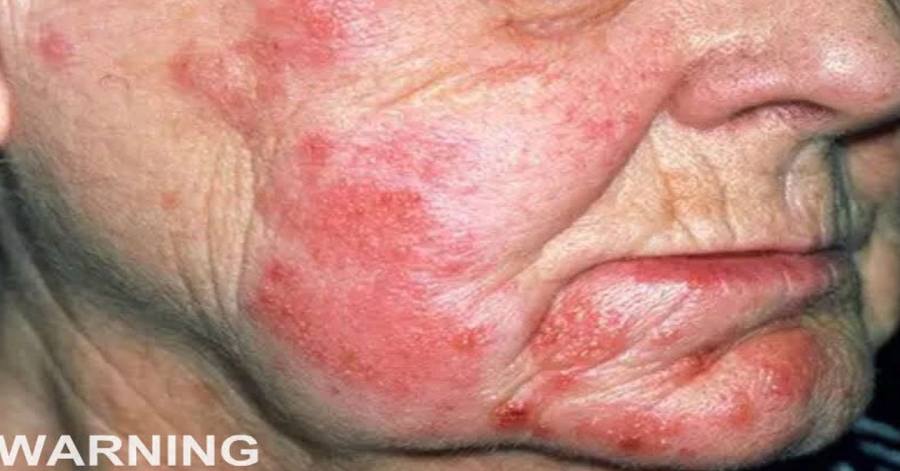
Shingles, also known as herpes zoster, is a disease that often causes confusion and concern, largely because many people are unaware of its origin, true causes, and why it can appear even in those who seem perfectly healthy. Although not always widely discussed, shingles is relatively common, especially after a certain age, and understanding it is key to acting promptly and avoiding complications.
Shingles is neither new nor mysterious. It is directly caused by the varicella-zoster virus, the same virus responsible for chickenpox in childhood. What many don’t realize is that after chickenpox resolves, the virus does not leave the body. Instead, it remains dormant for years or even decades within the nervous system, causing no symptoms. Under certain circumstances, it can reactivate and lead to shingles. This reactivation typically occurs when the immune system is weakened—whether by the natural aging process, prolonged stress, chronic illnesses, medical treatments that suppress immunity, or periods of intense physical or emotional strain. While shingles is more common in adults over 50, younger people can also be affected.
One of the most characteristic features of shingles is that it rarely appears without warning. Early symptoms are often nonspecific and easily mistaken for other conditions: localized pain, burning, tingling, or hypersensitivity in a specific area of the body. These sensations can emerge days before any visible rash, making early diagnosis difficult. As the illness progresses, a localized rash typically appears, usually on just one side of the body. This one-sided pattern reflects the virus reactivating along a specific nerve, which explains why the lesions follow a defined distribution rather than spreading everywhere. Although the rash is striking, specialists emphasize that the associated pain can be the most intense and persistent symptom.
With appropriate medical treatment, most cases of shingles resolve favorably. Antiviral medications, when started within the first 72 hours of symptom onset, can shorten the illness and reduce the risk of complications. However, when diagnosis is delayed, one of the most feared long-term effects may develop: postherpetic neuralgia—persistent pain lasting months or even years after the rash disappears. This chronic pain, often described as a constant burning or stabbing sensation, interferes with sleep, rest, and daily activities, affecting both
quality of life and emotional well-being. For this reason, doctors stress the importance of not dismissing early symptoms and seeking medical advice as soon as shingles is suspected.
Another common question is whether shingles is contagious. The answer is only partly yes. A person with shingles does not transmit shingles itself, but they can transmit the varicella-zoster virus to someone who has never had chickenpox or the chickenpox vaccine, causing chickenpox—not shingles. Therefore, during the active phase, it is recommended to avoid direct contact with immunocompromised individuals, pregnant women, and newborns.
In recent years, prevention has become paramount. Vaccines specifically designed to reduce the risk of developing shingles—and to lessen the severity if it does occur—are now available. Health organizations recommend vaccination primarily for older adults and people with risk factors, as it has proven effective in preventing complications. Beyond treatments and vaccines, shingles offers a clear lesson: health depends not only on the absence of visible illness. A balanced immune system, stress management, and attention to the body’s signals all play fundamental roles. Often, the body gives warning signs long before a problem becomes obvious.
In short, shingles is a well-known but often underestimated disease. Understanding its origin, recognizing its early symptoms, and acting promptly can significantly alter its course. Being informed does not cause alarm—it enables prevention, and in this case, vigilance can help avoid prolonged pain and unnecessary complications.