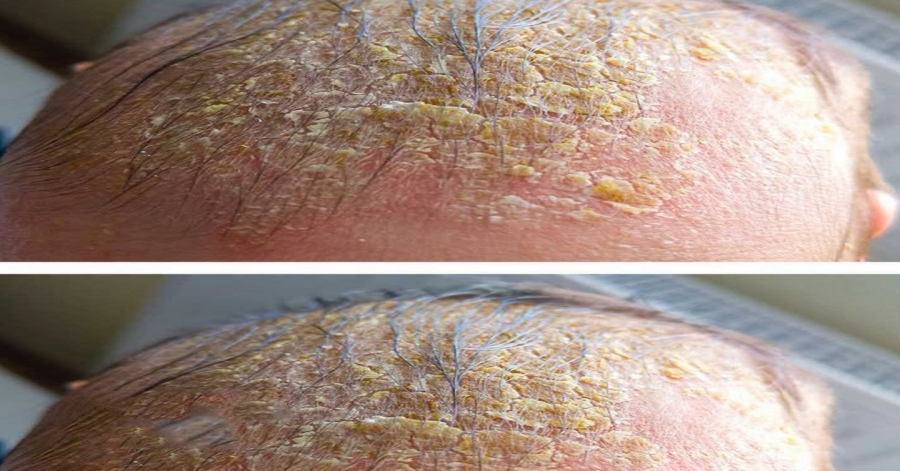
An oozing yellow crust on the scalp can be uncomfortable and worrying, especially if it doesn’t seem to heal. While long waitlists for medical appointments are frustrating, understanding possible causes and home care strategies can offer reassurance and direction. This article outlines the main reasons behind this condition, practical steps for relief, and guidance on when to consult a professional.
**What Is the Yellow Crust?**
The yellow crust forms when fluid from skin irritation or infection dries on the scalp. A yellow color often indicates pus, signaling infection or inflammation. Pay attention to the size of the affected area, how often it oozes, and any accompanying symptoms like itching or pain. Measuring the area (in centimeters or inches) can help when you finally speak with a healthcare provider.
**Common Causes**
Several conditions can lead to a yellow crust on the scalp:
- **Seborrheic dermatitis** – red, flaky patches that may ooze and crust.
- **Psoriasis** – a chronic autoimmune condition causing thick, scaly patches.
- **Folliculitis** – inflamed hair follicles due to bacterial or fungal infection, leading to pustules that crust over.
- **Impetigo** – a highly contagious bacterial infection (Staphylococcus aureus or Streptococcus pyogenes) common in children but also affecting adults. It starts as red sores or blisters that burst, leaving a thick, golden-yellow crust. Impetigo spreads easily through close contact and is more likely if you have cuts or abrasions.
**Symptoms to Watch For**
Seek medical attention if you experience:
- Persistent itching, redness, swelling, or pain.
- Spreading or worsening of the crust.
- Systemic signs like fever, fatigue, or swollen lymph nodes (which may indicate the infection has spread).
Also consult a doctor if the crust lasts more than a week without improvement, if you notice increasing warmth or pus, or if you have significant hair loss or considerable discomfort.
While waiting to see a doctor, you can try:
- Applying a warm, damp cloth to soften the crust and soothe irritation.
- Gentle cleansing with a mild, fragrance-free shampoo.
- Diluted
tea tree oil (do a patch test first) for its antimicrobial properties.
- Coconut oil to hydrate the scalp and reduce flaking.
**Over-the-Counter Treatments**
Depending on the likely cause:
- Anti-dandruff shampoos with zinc pyrithione, selenium sulfide, or ketoconazole help with seborrheic dermatitis and mild fungal infections.
- Topical antibiotic creams (bacitracin or neomycin) if a bacterial infection is suspected.
- Hydrocortisone cream to reduce inflammation and itching (use sparingly and briefly).
**Be Cautious with Viral Hacks**
Social media remedies like apple cider vinegar or baking soda can disrupt the skin’s natural pH and cause further irritation. Always consult a professional before trying unconventional treatments.
**Hygiene and Prevention**
- Wash hair regularly with a gentle shampoo to remove excess oil and dead skin cells.
- Avoid sharing combs, hats, pillowcases, or towels to prevent spreading infection.
- To reduce future flare-ups: manage stress, eat a balanced diet rich in vitamins and minerals, avoid harsh hair products, and protect your scalp from excessive sun exposure.
**Navigating Long Clinic Waitlists**
While waiting for an in-person appointment:
- Consider a virtual consultation for timely advice and possible prescriptions.
- Keep a symptom log with photos and measurements. This documentation helps your provider make a faster, more accurate diagnosis.
Remember: many scalp conditions are manageable with proper care. Being informed and proactive can ease discomfort and improve outcomes while you await professional assessment.